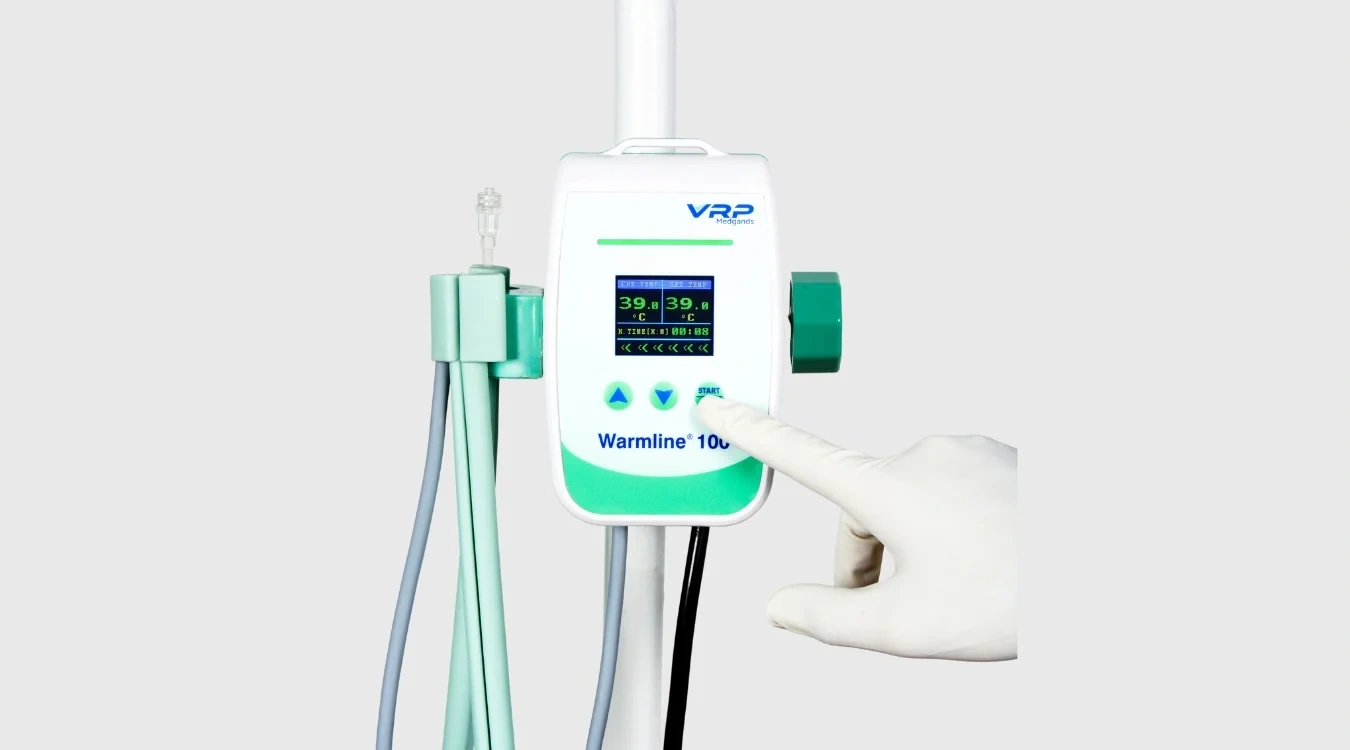
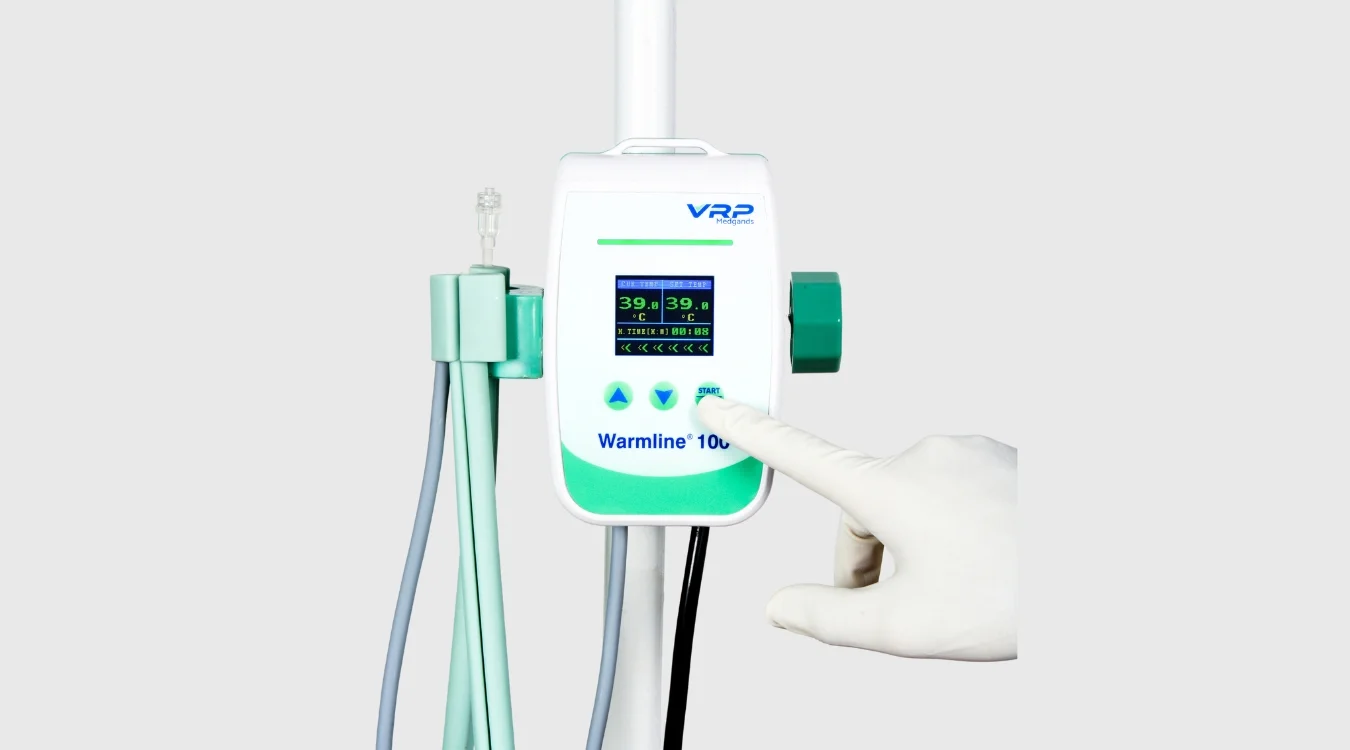
What is a blood and fluid warmer?
A blood and fluid warmer is a certified medical device that heats intravenous (IV) fluids, blood products, and irrigation fluids to a safe physiological temperature — between 37°C and 42°C — before administration to a patient. In 2026, blood and fluid warmers are considered the <strong>gold standard for preventing iatrogenic hypothermia</strong> during surgery, trauma resuscitation, and intensive care. This page covers the 7 primary clinical uses, how to choose the right warmer for your facility, and why dry-heat open-system technology like the Warmline® 100 is rapidly replacing traditional water-bath systems in hospitals across India.
On this page:
- 1. Why blood warming matters
- 2. 7 clinical uses of blood and fluid warmers
- 3. Risks of not warming IV fluids
- 4. Dry heat vs. water bath comparison
- 5. How to choose a blood warmer for your hospital
- 6. Safety standards and certifications
- 7. Frequently asked questions
Why would you use a blood warmer?
The primary goal is to maintain normothermia. When cold fluids are infused directly into the bloodstream, they can cause a rapid drop in core body temperature, leading to a dangerous condition known as accidental hypothermia.
7 Clinically Proven Benefits of Blood and Fluid Warmer
Maintaining normothermia (approximately 37°C) is a key physiological parameter that directly impacts patient outcomes and hospital efficiency.
- 1. Reduced Risk of Surgical Site Infections (SSI)
Maintaining patient body temperature improves tissue oxygenation and immune response, significantly reducing the risk of post-operative infections, as supported by clinical studies.
- 2. Reduced Blood Loss and Improved Coagulation
Hypothermia negatively affects platelet function and coagulation pathways. Warming blood and IV fluids supports normal clotting and helps reduce intraoperative blood loss.
- 3. Improved Cardiac Stability
Cold fluid infusion can trigger arrhythmias, particularly in elderly or high-risk patients. Blood and fluid warmers ensure temperature-controlled delivery, reducing cardiac stress.
- 4. Faster Post-Operative Recovery
Patients whose body temperature is maintained during surgery often recover from anesthesia more efficiently, leading to shorter PACU stays and improved post-operative stability.
- 5. Prevention of the Trauma “Lethal Triad”
In trauma care, fluid warming helps prevent the progression of hypothermia, acidosis, and coagulopathy, a combination associated with increased mortality.
- 6. Protection Against Hemolysis
Modern dry-heat warming technologies incorporate dual-sensor temperature monitoring to prevent overheating, helping preserve red blood cell integrity during transfusion.
- 7. Long-Term Cost Efficiency for Hospitals
By reducing complications, ICU admissions, and infection-related treatments, blood and fluid warmers contribute to measurable long-term cost savings for healthcare facilities.
What Happens if IV Fluids Are Not Warmed?
Administering unwarmed blood or IV fluids — typically stored at 4°C — directly into a patient's bloodstream can trigger a cascade of life-threatening complications known as the "Lethal Triad":
- Hypothermia — Core body temperature drops below 35°C, impairing organ function and slowing drug metabolism.
- Coagulopathy — Cold temperatures impair clotting factor activity, causing uncontrollable bleeding even in the presence of adequate blood products.
- Acidosis — Reduced tissue perfusion causes metabolic acidosis, further worsening cardiac function.
According to PubMed-indexed research, perioperative hypothermia increases the risk of surgical site infections (SSI) by up to 300% and can extend ICU stay by 1–2 days on average. The NICE CG65 guideline mandates active warming for all surgical patients undergoing procedures longer than 30 minutes — and fluid warming is a core component of that protocol.
For trauma patients receiving massive transfusions (>10 units of PRBCs), unwarmed blood can rapidly cause cardiac arrhythmia and cardiac arrest. This is why fluid warming in the emergency room is not optional — it is a life-saving clinical standard.
How to Choose a Blood and Fluid Warmer for Your Hospital
Hospital procurement managers and clinical engineers should evaluate blood warmers against these 5 criteria:
- Open vs. Closed System — Open-system warmers (like the Warmline® 100) work with any standard universal IV set. Closed systems require costly proprietary disposable kits — increasing recurring operational cost by ₹5,000–₹15,000 per month per unit.
- Warming Technology — Dry-heat systems eliminate waterborne contamination risk (Pseudomonas, biofilm) associated with traditional water-bath warmers. Essential for OT and NICU environments.
- Temperature Precision and Safety Alarms — Look for dual-sensor systems that maintain fluid temperature between 37°C–42°C and trigger audible + visual alarms if the limit is exceeded. This is mandatory per IEC 60601-1-2.
- Regulatory Compliance — In India, ensure the device is CDSCO registered and carries ISO 13485:2016 and ASTM F2172 certification. Non-certified devices carry legal and patient safety risk.
- Portability & Mounting — For ICUs and emergency bays, choose a compact unit that mounts on a standard IV pole and can be repositioned without tools. For ambulance/EMS use, battery-independent portable models are preferred.
Key Uses of Blood and Fluid Warming Systems
-
A. Emergency and Trauma Care (ER Fluid Warmer)
In trauma situations, patients often require massive blood transfusions. Using an ER fluid warmer ensures that large volumes of blood can be delivered rapidly without causing cardiac arrhythmia or "cold shock" to the patient’s system.
-
B. Surgical & Perioperative Care
During surgery, anesthesia impairs the body's ability to regulate heat. Maintaining fluid warming protocols during long procedures reduces the risk of surgical site infections (SSI) and helps patients wake up faster from anesthesia.
-
C. Intensive Care Units ( ICU ) & Neonatal Units
In the ICU, continuous fluid warming is used for critically ill patients to prevent metabolic stress. In neonatal care, it is a life-saving measure to protect newborns who cannot yet regulate their own body heat.
-
D. Operating Theatres (OT)
Used during surgical procedures longer than 30 minutes to maintain normothermia and reduce anesthesia-related complications.
-
E. Neonatal & Pediatric Units
Infants are highly vulnerable to heat loss; even small volumes of cold IV fluids can cause dangerous drops in body temperature.
-
F. Ambulance & EMS
Portable blood and fluid warmers (like the Warmline 100) help stabilize trauma patients during the "Golden Hour" of transport.
Comparison: Dry Warming vs. Traditional Methods
| Feature | Dry Warming Systems (Warmline 100) | Traditional Water Baths |
|---|---|---|
| Warming Technology | Open System (No disposables) | Closed (Requires proprietary kits) |
| Contamination Risk | None (Dry Heat) | High (Water-borne bacteria) |
| Heating Speed | Rapid & Consistent | Slow & Uneven |
| Infection Control | Superior (Zero water risk) | High (Risk of biofilm/bacteria) |
| Operational Cost | Zero recurring costs | High (Costly disposable sets) |
| Setup Time | Less than 2 Minutes (Snap-and-go) | 5-10 Minutes (Water heating) |
| Compatibility | All Standard IV Sets | Brand-specific sets only |
| Maintenance | Low Maintenance | High (Regular Cleaning) |
Top Reasons to Choose VRP Medgands Fluid Warmers
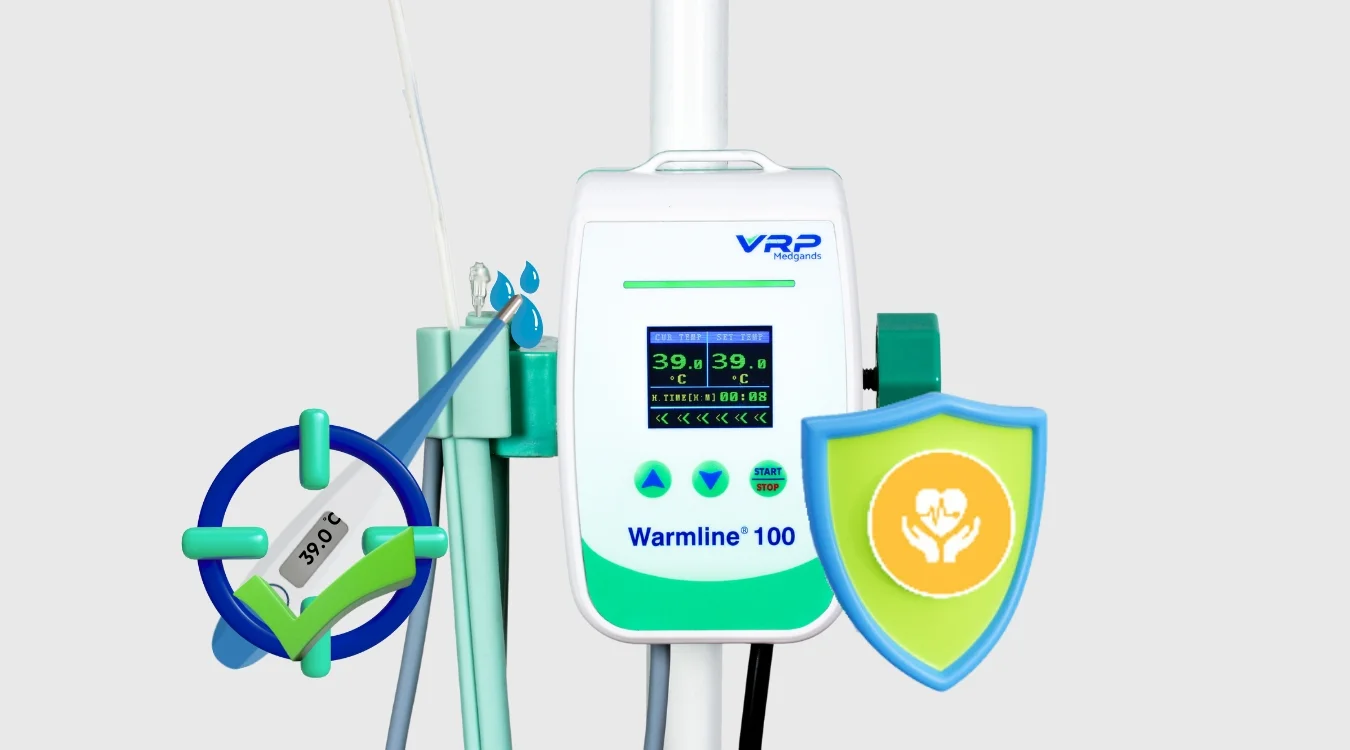
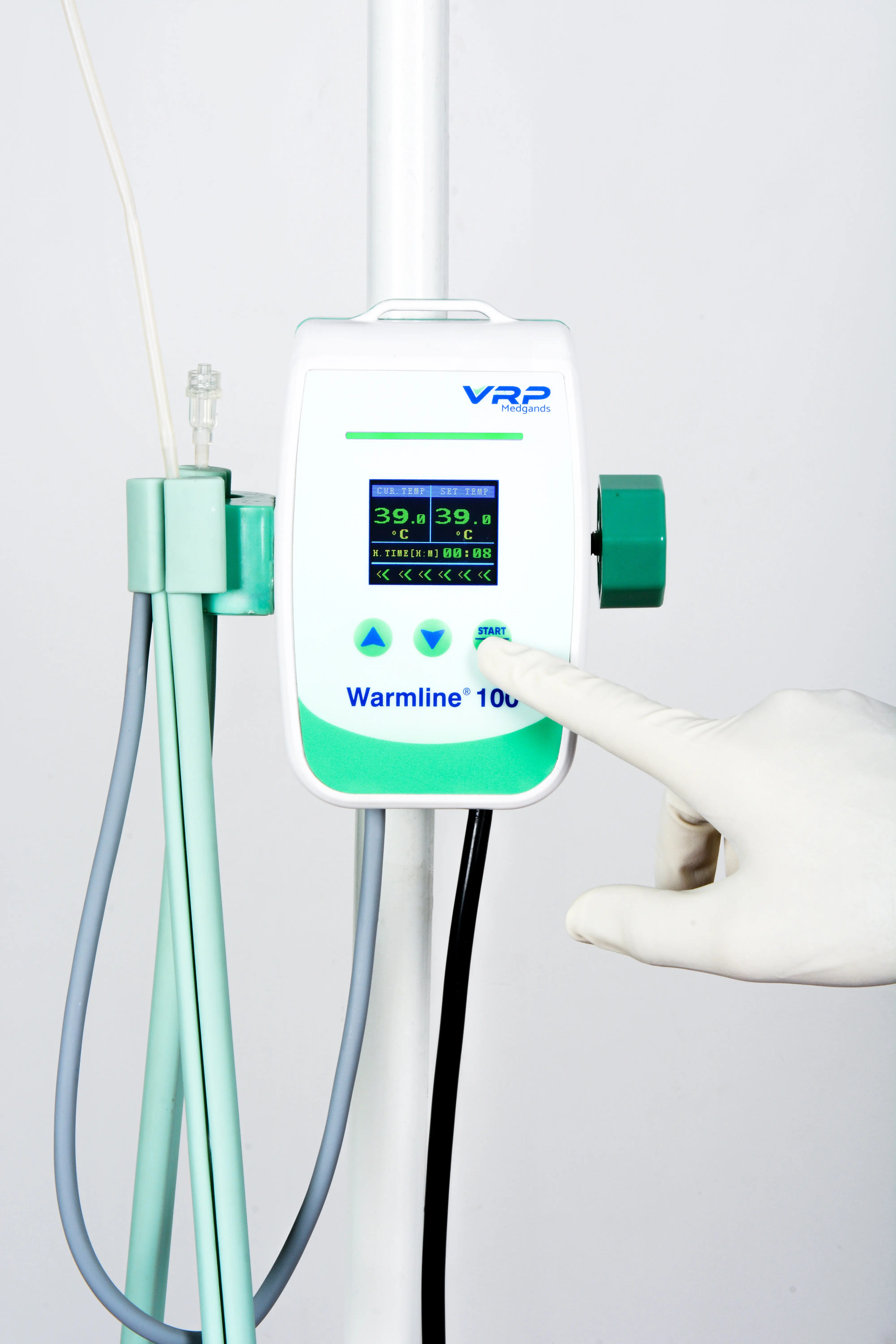
- Precision Sensors: Our systems answer the "why" by providing real-time digital feedback, ensuring fluids never exceed the safe 42°C limit.
- Portability: Ideal for emergency response and field hospitals.
- Safety Alarms: Visual and acoustic alarms for overheating or system errors.
Safety Standards and Trust
Healthcare facilities should prioritize blood and fluid warmers that align with recognized safety and performance standards:
- IEC 60601-1-2 (4th Edition)
Ensures electromagnetic compatibility in operating rooms and ICU environments. - Dry-Heat Warming Technology
Eliminates infection risks associated with older water-bath warming systems. - Intelligent Safety Alarms
Audible and visual alerts for over-temperature (>42°C), flow interruption, or system malfunction.

Clinical References
- NCBI / PubMed: Impact of perioperative hypothermia on patient outcomes
- The Lancet: Thermal management and infection risk in surgical patients
- NICE Guidelines (CG65): Hypothermia – prevention and management in adults undergoing surgery
Medical Disclaimer
This content is intended for healthcare professionals, hospital administrators, and medical equipment procurement teams. It is provided for informational purposes only and does not constitute medical advice. Clinical decisions should always follow institutional protocols, manufacturer instructions, and applicable medical guidelines.
Blogs Related to Blood and Fluid Warmer
-
2026 Hospital Procurement Guide: Choosing the Right Warmer: A complete checklist for purchase managers, focusing on CDSCO compliance and "Open System" cost savings.
-
Preventing Hemolysis: The Science of Temperature Precision: Deep dive into why the 42°C threshold is critical and how Silicon Heating Technology protects blood integrity.
Asked Questions
1. What is the primary use of a blood and fluid warmer?
The primary use is to prevent accidental perioperative hypothermia by warming refrigerated blood and IV fluids to a safe physiological temperature (37°C to 42°C) before infusion. This is critical in surgery, trauma care, and ICUs to maintain patient normothermia and stabilize metabolic rates.
2. Can platelets or blood products go through a fluid warmer?
Yes, but with strict temperature control. While packed red blood cells (PRBCs), crystalloids, and colloids are commonly warmed, platelets must be handled carefully. Our Warmline 100 uses precision dry-heat technology to ensure all compatible blood products are warmed without the risk of hemolysis (cell damage) or overheating beyond the 42°C safety limit.
3. Why is blood warming necessary in clinical settings?
Infusing cold fluids can lead to coagulopathy (impaired blood clotting) and cardiac arrhythmias. Blood warming is necessary to keep the heart rate stable during rapid infusions and to prevent the "Lethal Triad" in trauma patients: acidosis, coagulopathy, and hypothermia.
4. What is a "Hotline" blood and fluid warmer?
A "Hotline" or "Warmline" refers to a point-of-care warming system that heats fluids as they flow through the IV line. Unlike traditional water baths, modern systems like the Warmline series are "Open Systems," meaning they are compatible with standard universal IV sets, offering a more flexible and hygienic solution for busy hospitals.
5. Is it safe to warm up IV fluids at home?
No. IV fluids should never be warmed at home using microwaves or hot water, as this leads to uneven heating and can cause fatal thermal injury or gas embolisms. Medical-grade warmers at VRP Medgands use dual-sensor technology to provide consistent, monitored heat that meets 2026 clinical safety standards.
6. Is dry heat safer than water-bath warming?
Absolutely. Dry heat technology, as seen in the Warmline 100, eliminates the risk of cross-contamination and waterborne pathogens like Pseudomonas. This makes it the safer, low-maintenance choice for sterile environments like the Operation Theatre (OT) and NICU.
About VRP Medgands
VRP Medgands is a leading ISO-certified medical device manufacturer based in Chennai, India. For over 17 years, we have specialized in high-performance thermal management solutions, including the Warmline® series of patient warmers. Our mission is to support perioperative safety and normothermia in OTs and ICUs across the globe.
Certifications: ISO 13485:2016, CDSCO Certified, NABL Approved, IEC 60601-1, IEC 60601-1-2, ASTM F2172.
Headquarters: No 54/11, 1st Floor, 4th Street, Rukmani Nagar, Poonamallee, Chennai - 600056
Contact: +91 44 3594 6000 | +91 9962145127 | enquiry@vrpmedgands.com | vigneshn@vrpmedgands.com